L
et’s be blunt: If you’re handling Protected Health Information (PHI) and not doing regular HIPAA risk assessments, you’re basically driving without insurance during a hailstorm. One bad crash and you’re looking at fines up to $1.5 million per violation category—yes, that’s the current maximum.
But here’s the good news: Passing your HIPAA risk assessment isn’t rocket science. It’s about systematically checking boxes before the government does it for you. Let’s walk through exactly what you need in 2026.
What Actually Is a HIPAA Risk Assessment? (No Legalese, Promise)
Think of it as a “security physical” for your organization. The Health Insurance Portability and Accountability Act (HIPAA) requires you to:
- Identify where PHI lives and travels in your organization
- Spot vulnerabilities that could expose it
- Implement safeguards to protect it
- Document everything (because if it’s not written down, it didn’t happen)
Quick reality check: 93% of healthcare organizations experienced a data breach in the past 3 years, with average costs reaching $10.93 million according to IBM’s 2023 Cost of a Data Breach Report.
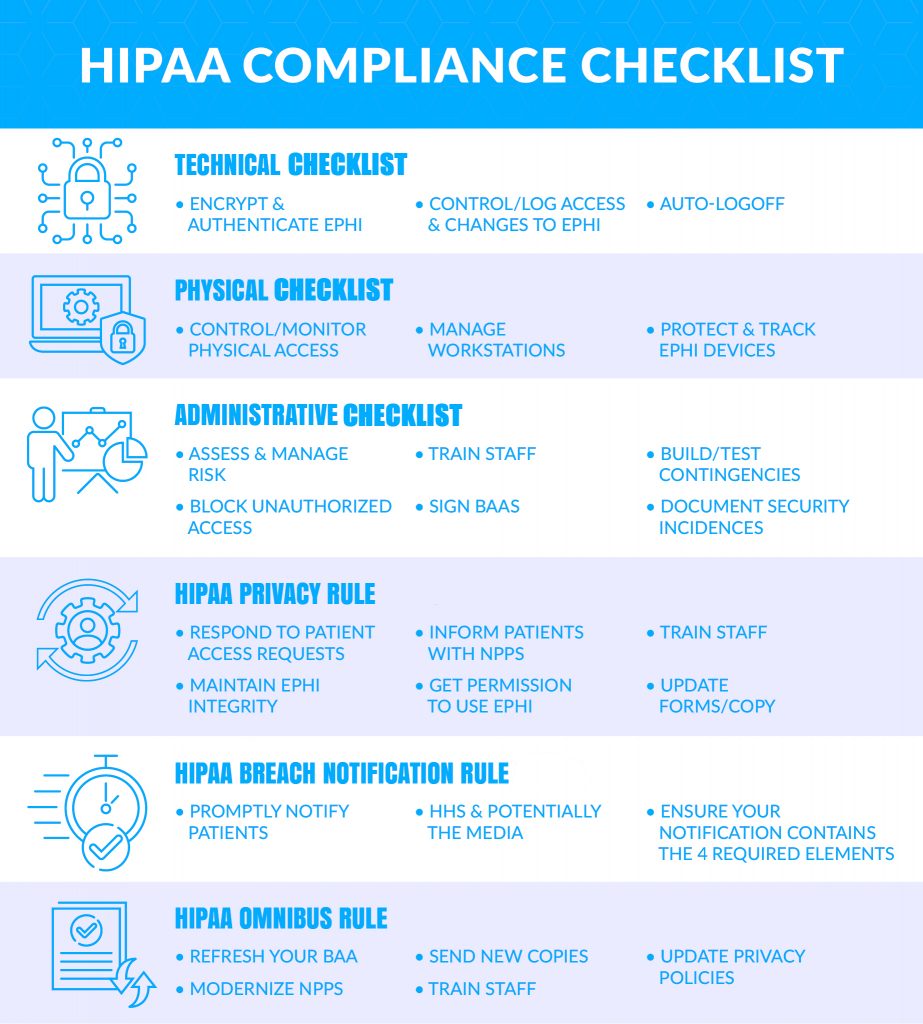
Your 2026 HIPAA Risk Assessment Checklist
Technical Safeguards (The Digital Lockdown)
These protect your electronic PHI (ePHI). Check each box you’ve implemented:
✅ Access Control: Unique user IDs, automatic logoff after 15 minutes of inactivity, and emergency access procedures documented.
✅ Encryption: All ePHI encrypted both at rest (storage) and in transit (email, transfers). Pro tip: Use AES-256 encryption—it’s the gold standard.
✅ Audit Controls: Systems track who accessed what PHI, when, and from where. Logs retained for at least 6 years (yes, really).
✅ Integrity Controls: Digital signatures or checksums prevent unauthorized alteration of PHI.
✅ Transmission Security: VPNs for remote access, TLS 1.2+ for web applications, and encrypted messaging for clinical communication.
Common gap: 43% of healthcare organizations don’t encrypt all mobile devices containing PHI. That’s like leaving patient files in an unlocked car.
Physical Safeguards (The Actual Lockdown)
PHI isn’t just digital—it’s also in filing cabinets, workstations, and that sticky note on Jane’s monitor.
✅ Facility Access Controls: Badge entry systems, visitor logs, and separate secure areas for PHI storage.
✅ Workstation Security: Computer screens facing away from public view, privacy filters on monitors, and clear-desk policies enforced.
✅ Device & Media Controls: Inventory of all devices containing PHI, encryption on laptops/tablets, and proper destruction procedures (shredding, degaussing).
✅ Disposal Procedures: PHI shredded or securely erased before disposal. No tossing patient records in recycling!
Real story: A clinic was fined $300,000 for leaving 71 boxes of patient records in a physician’s backyard. Physical safeguards matter.
Administrative Safeguards (The Human Firewall)
Your people are both your biggest vulnerability and strongest defense.
✅ Risk Analysis Documentation: Formal risk assessment performed annually (and after any major system change).
✅ Security Officer: Designated HIPAA Security Officer with documented responsibilities.
✅ Employee Training: Annual HIPAA training with attendance records. Include password hygiene and phishing recognition.
✅ Incident Response Plan: Clear steps for breach notification (required within 60 days of discovery).
✅ Business Associate Agreements: Signed BAAs with every vendor touching PHI—yes, including your cloud storage provider.
✅ Policies & Procedures: Written, accessible, and actually followed. Update them at least annually.
The 5 Most Overlooked Items (That Get Organizations Fined)
- Mobile Device Management: That doctor checking patient emails on her personal phone? If it’s not encrypted and remotely wipeable, you’re vulnerable.
- Email Encryption: Sending PHI via regular email is like mailing a postcard with lab results. Use encrypted email or secure portals.
- Password Policies: “Password123” doesn’t cut it. Require 12+ characters, multi-factor authentication, and regular changes.
- Paper Records: Digital gets attention, but paper charts left at nursing stations cause 24% of breaches.
- Vendor Management: Your EHR vendor gets hacked? You’re still liable if you didn’t have a BAA and verify their security.
How Often Should You Do This?
- Full assessment: Annually (required)
- Mini-assessment: After any major change (new EHR, office move, merger)
- Spot checks: Quarterly for high-risk areas
Pro tip: Use the NIST Cybersecurity Framework as your guide—it’s what OCR auditors increasingly reference.
“We Found Gaps—Now What?”
Don’t panic. The Office for Civil Rights (OCR) cares more about good faith effort than perfection. Document:
- The vulnerability found
- Your remediation plan
- The timeline for fixing it
- Why certain risks were accepted (if applicable)
This “recognize and respond” approach shows due diligence even if you’re not 100% perfect.
Free Resources That Actually Help
- OCR’s Security Risk Assessment Tool: Free tool from HHS
- NIST HIPAA Security Toolkit: Comprehensive guidance
- HHS Breach Portal: See real cases and learn from others’ mistakes
When to Call Professionals
Consider expert help if:
- You’re a small practice without IT staff
- You’ve had a breach or near-miss
- You’re implementing new technology
- An audit notice arrives
Our healthcare compliance team has helped 200+ organizations pass assessments and avoid fines. Sometimes an outside perspective spots what you’ve been missing.
The Bottom Line
HIPAA compliance isn’t about being perfect—it’s about being diligent. Regular risk assessments aren’t bureaucratic paperwork; they’re your organization’s immune system against devastating breaches and fines.
The question isn’t “Can we afford to do this?” It’s “Can we afford not to?”